CTEPH Case Study 2
63-year-old man with progressively worsening dyspnea on exertion (DOE) over last 3 months
-
Moderately active—had walked 30+ mins/day—until recent progression of dyspnea
-
History of acute pulmonary embolism (PE) subsequent to appendectomy 15 years previous
-
History of splenectomy for hereditary spherocytosis
-
Body mass index (BMI): 31 kg/m2; weight: 238 lbs
Echocardiogram
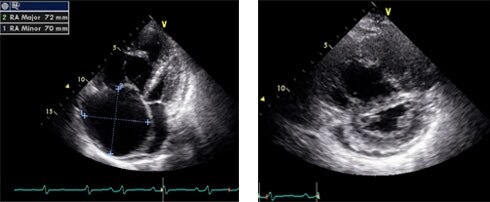
Additional studies
-
No evidence of acute PE on computed tomographic pulmonary angiogram (CTPA)
-
N-terminal prohormone of brain natriuretic peptide (NT-proBNP): 1439 pg/mL
-
6-minute walk distance (6MWD): 398 meters
-
Assessed as WHO Functional Class II/III
Right heart catheterization
-
Mean pulmonary arterial pressure (mPAP): 48 mmHg
-
Right atrial pressure (RAP): 9.5 mmHg
-
Pulmonary capillary wedge pressure (PCWP): 9.8 mmHg
-
Cardiac output (CO): 3.1 L/min
-
Cardiac index (CI): 1.9 L/min/m2
-
ulmonary vascular resistance (PVR): 792 dyn∙sec∙cm-5
Key takeaways
Patients with confirmed PH should have a V/Q scan to rule out potentially curable (via pulmonary thromboendarterectomy) CTEPH1
A V/Q scan showing perfusion defects should prompt referral to an experienced center for further evaluation and, if CTEPH is confirmed, operability assessment1
References:
1. Kim NH, Delcroix M, Jenkins DP, et al. Chronic thromboembolic pulmonary hypertension. J Am Coll Cardiol. 2013;62(suppl D):D92-D99.


