CTEPH pathophysiology
CTEPH can result from PE1
CTEPH can be the result of a single pulmonary embolism (PE) or recurrent pulmonary emboli arising from sites of venous thrombosis.1
According to the widely held “embolic hypothesis,” these PE result in endothelialized residua that obstruct or significantly narrow pulmonary arteries.2
The reduced bioavailability of endogenous vasodilators, like nitric oxide, may contribute to endothelial dysfunction3
The development of distal, small-vessel arteriopathy may also contribute to pulmonary hypertension (PH) and right ventricular overload
Small vessel arteriopathy is characterized by medial hypertrophy, intimal proliferation and thickening, microthrombi formation, and plexiform lesions4
The pathogenesis of this arteriopathy remains unclear1
Previous venous thromboembolic disease has also been linked to development of CTEPH5
CTEPH can be easy to diagnose if you’re aware of the distinguishing factors.6
Features of pulmonary vasculature in CTEPH4
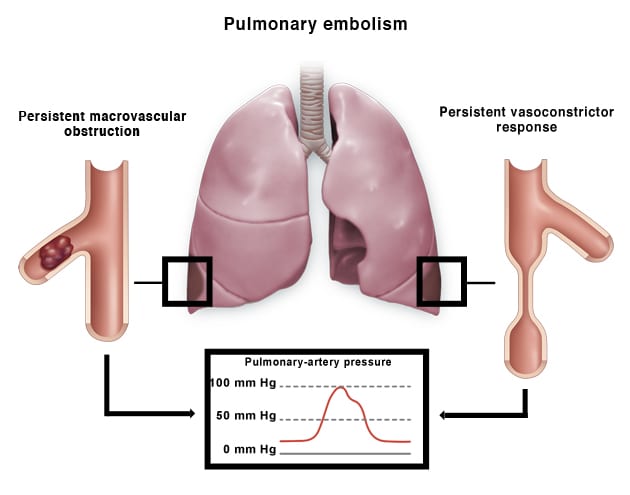
CTEPH results from persistent macrovascular obstruction and a vasoconstrictor response that lead to a secondary small-vessel arteriopathy. Reductions in the pulmonary-artery diameter due to thrombosis and vasoconstriction result in adverse vascular remodeling.4
Pulmonary embolism4
Pulmonary hypertension4
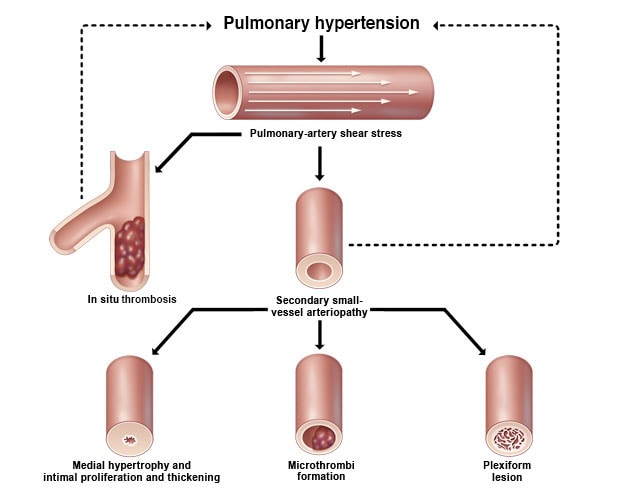
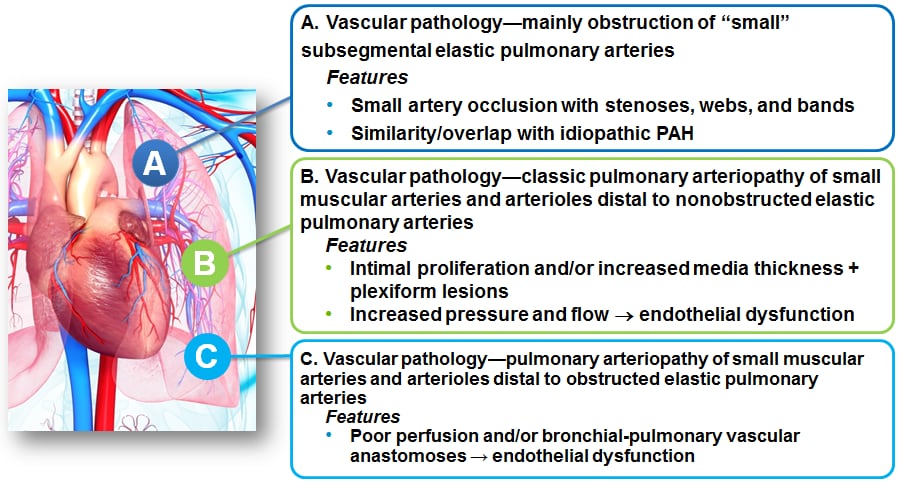
Multiple mechanisms of small-vessel disease are operative in CTEPH7
Microvascular disease in CTEPH may adversely impact selection for pulmonary thromboendarterectomy (PTE) surgery (also called pulmonary endarterectomy [PEA]) or may affect surgical outcomes.7
CTEPH is not pulmonary arterial hypertension (PAH)
Distinguishing CTEPH from PAH (WHO Group 1 PH) is essential.
CTEPH is caused by macrovascular obstructions in the pulmonary arteries.4 In appropriate surgical candidates, such obstructions can be removed via PTE surgery and potentially cure CTEPH.6
PAH is not caused by macrovascular obstructions and cannot be treated with PTE surgery. Though there is no cure for PAH, it can be effectively managed with medical therapies.2
All patients in whom PH is suspected should have a ventilation/perfusion (V/Q) scan to exclude CTEPH.6 Patients who are already diagnosed with other forms of PH but who have not had a V/Q scan should get one to exclude CTEPH.6
References:
1. Fedullo P, Kerr KM, Kim NH, Auger WR. Chronic thromboembolic pulmonary hypertension. Am J Respir Crit Care Med. 2011;183(12):1605-1613. 2. Humbert M. Pulmonary arterial hypertension and chronic thromboembolic pulmonary hypertension: pathophysiology. Eur Respir Rev. 2010;19:59-63. 3. Skoro-Sajer N, Mittermayer F, Panzenboeck A, et al. Asymmetric dimethylarginine is increased in chronic thromboembolic pulmonary hypertension. Am J Respir Crit Care Med. 2007;176(11):1154-1160. 4. Piazza G and Goldhaber SZ. Chronic thromboembolic pulmonary hypertension. N Engl J Med. 2011;364:351-360. 5. Bonderman D, Wilkens H, Wakounig S, et al. Risk factors for chronic thromboembolic pulmonary hypertension. Eur Respir J. 2009;33:325-331. 6. Kim NH, Delcroix M, Jenkins DP, et al. Chronic thromboembolic pulmonary hypertension. J Am Coll Cardiol. 2013;62(suppl D):D92-D99. 7. Galiè N and Kim NH. Pulmonary microvascular disease in chronic thromboembolic pulmonary hypertension. Proc Am Thorac Soc. 2006;3(7):571-576.


